ANTIBIOTIC THERAPY
Amoxicillin or Amoxicillin + Clavulanic Acid
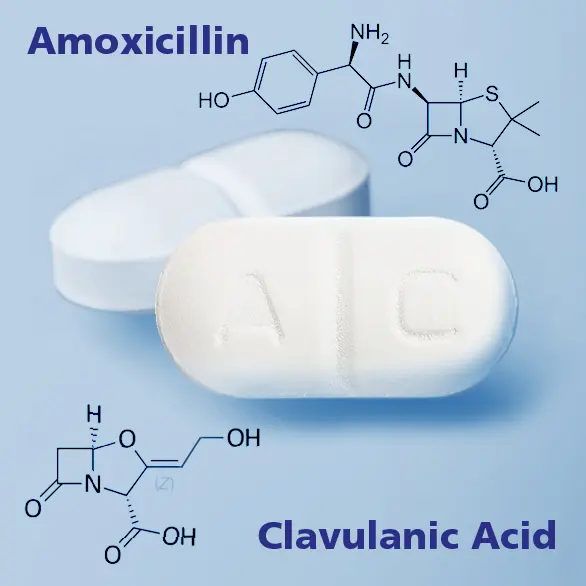
Since their discovery, antibiotics are a fundamental tool in medicine. Their use is very important, sometimes indispensable, to eradicate infections of bacterial origin, both in children and in adults, therefore they are to be considered real life-saving drugs.
There are several types of antibiotics. The family of beta-lactam antibiotics certainly includes a large portion of those most prescribed and used by patients all over the world.
The most used beta-lactam antibiotic is undoubtedly Amoxicillin, capable of inhibiting the synthesis of key enzymes for the synthesis of peptidoglycan, a structural component of the bacterial cell wall. Thanks to this mechanism of action, Amoxicillin is able to kill various types of bacteria.
Amoxicillin is the drug of first choice in the treatment of various bacterial infections. First, we can list respiratory tract infections, but also ENTl, stomatological, urogenital, skin, gastrointestinal infections, septicemia, and postoperative sepsis.
Unfortunately, some bacteria have developed powerful mechanisms of resistance to Amoxicillin and are able to inactivate it (by breaking the beta-lactam ring that distinguishes its chemical structure). For this reason, Amoxicillin + Clavulanic acid, better known under the commercial name of Augmentin®, was formulated, which improves the activity of the antibiotic by blocking the bacterial defense functions.